Why is good dental care important for your pet?
We know that your pet will benefit from good health the same way that you do; they will live longer, be more active and happy, and have a better quality of life. People who care about their pets understand this and are looking for the benefits of good veterinary care. Human dentistry developed as a distinct field of medicine to provide both preventive and problem-specific care. Anyone who knows the intense misery of a dental problem from a “toothache” or infected gums will tell you how desperate they were for relief from their pain, and how much they wished for a dentist to help them immediately. Vaccinations, good nutrition, parasite control, and advances in veterinary care are allowing pets to live many times longer than a dog, cat, horse, pet rabbit, or rodent living in the wild. Along with this longevity, the wide variety of breeds has contributed to the development of a number of dental diseases and problems.
The primary goals of veterinary dentistry are to have a pain-free comfortable mouth with normal function. Most pets are stoic and do not show pain therefore, the pain is often hidden. You can tell your dentist when your tooth hurts, but your pet can’t.
The most common symptoms of oral pain in a pet are increased mouth odor, otherwise known as “bad breath”, loss of playfulness, and increased sleeping to “get away” from the pain. Many pets show reluctance to eat dry food or chew treats they once enjoyed. Your pet will commonly act “old” when they have a painful mouth. Determining if the pet’s pain is related to the teeth and providing treatment will give your pet a new quality of life.
The most common health problem in dogs and cats is periodontal disease. This chronic infection of the gum tissue and jawbone commonly results in abscessed teeth that will have a “domino effect” on nearby teeth. Just like for our good oral health, your pet needs good home dental care, appropriate diet and treats, and regular care by your pet’s dental professional to help prevent periodontal disease. Twice yearly dental examinations by your veterinarian can detect problems early. Professional dental cleanings with full mouth dental x-rays are necessary as 60% of the tooth is located under the gumline. These are performed to assist in periodontal therapy if needed. Small dogs are much more commonly affected and seriously impacted by this hidden chronic infectious disease. Many pets suffer and lose teeth unnecessarily to this disease because regular preventive care gets “put off” until the future.
Good dental care is crucial to your pet’s health.
Dogs commonly suffer from fractured (broken) teeth that become infected, abscessed, and create chronic misery. Dogs break teeth by chewing or picking up hard objects including rocks, bones, metal objects, or nylon chew toys. Never let your dog chew on an object unless it is soft enough for you to bend it in your hands. There are only two ways to treat broken teeth to prevent them from developing tooth root abscesses in the jawbone. They can be saved with surgery or need to be extracted completely. Not providing care for these broken teeth results in lifelong pain for your pet.
Cats commonly develop resorptive lesions (a kind of cat cavity) that are very painful. Between 25% to 33% of all cats suffer silently from these hidden problems. Research has yet to find the cause of, or the way to prevent, these miserable lesions. Teeth that are affected by resorptive lesions need to be surgically removed to stop the pain.
Horses, rabbits, and rodents develop a unique set of dental problems due to the continuous growth, and uneven wear of their teeth. Care provided by a knowledgeable professional can vastly improve their quality of life and longevity.
Good dental care for your pet is a joint responsibility between you and your veterinarian. Daily home dental care, appropriate foods, and chew treats can help your pet at home. Your pet will need regular examinations and professional dental care when necessary to help prevent years of silent suffering with hidden chronic dental disease. Your pet will live years longer, have a happy life, and will return your love with big, wet, sweet-non-smelling kisses!
Pet Dental Cleanings
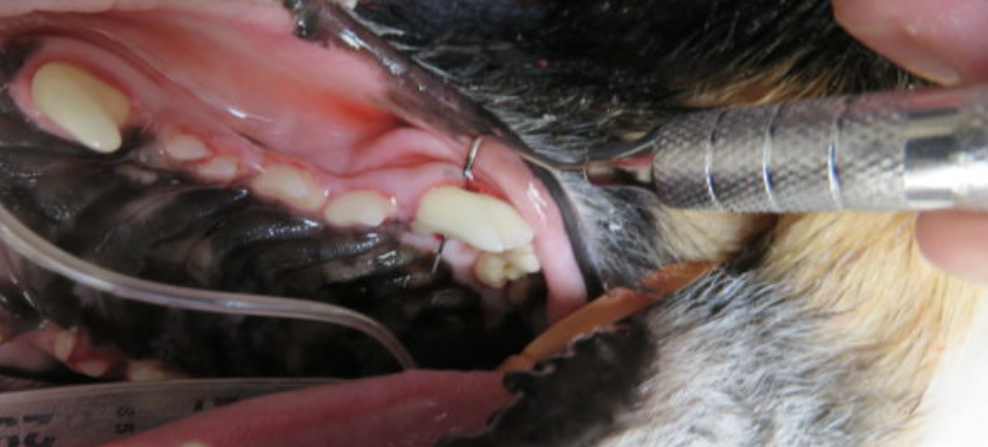
Dental Probing
Here at Lake County Veterinary Clinics, PLLC, we provide exceptional and comprehensive dental care for your pet, which is an important factor in living their best life, happy and healthy!
Professional Teeth Cleanings for both Dogs and Cats include the following:
- A comprehensive physical exam and oral exam as well as a consult to discuss oral pathology.
- Pre-Anesthesia Blood Work to assess organ function prior to anesthesia.
- General Anesthesia includes IV fluid therapy and monitoring. Your pet’s anesthesia will be individualized to their specific needs. All patients are monitored continuously on a multiparameter unit which monitors their heart rate, respiratory rate, CO2 levels, temperature, the electrical conductivity of the heart (EKG), and blood pressure. We make necessary changes with anesthesia to keep your pet safe during the procedure.
- *General anesthesia is required for all dental prophylaxis or any dental radiographs to ensure the airway is protected.
- Full mouth intraoral digital dental x-rays are obtained. These are obtained to evaluate for evidence of periodontal disease, fractured teeth, endodontic disease, assess for oral tumors, etc.
- Thorough professional periodontal therapy is performed.
- A thorough oral exam is performed under anesthesia to further assess for periodontal issues or other oral diseases.
- We send home a copy of medical records, dental charts, and discharge instructions for every patient.
Advanced Dental Care at Lake County Veterinary Clinics
Oral Surgery & Extractions
Extractions in a cat
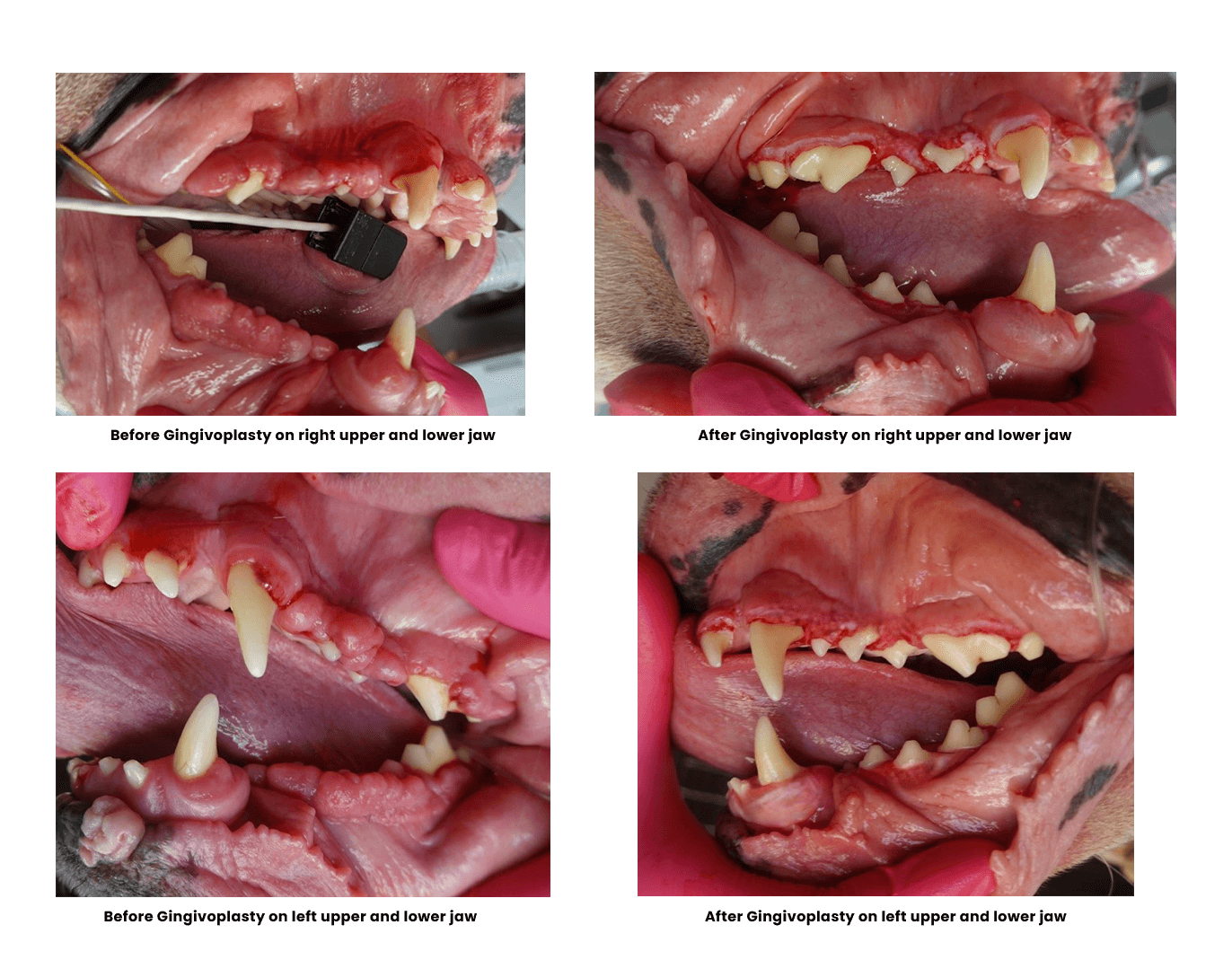
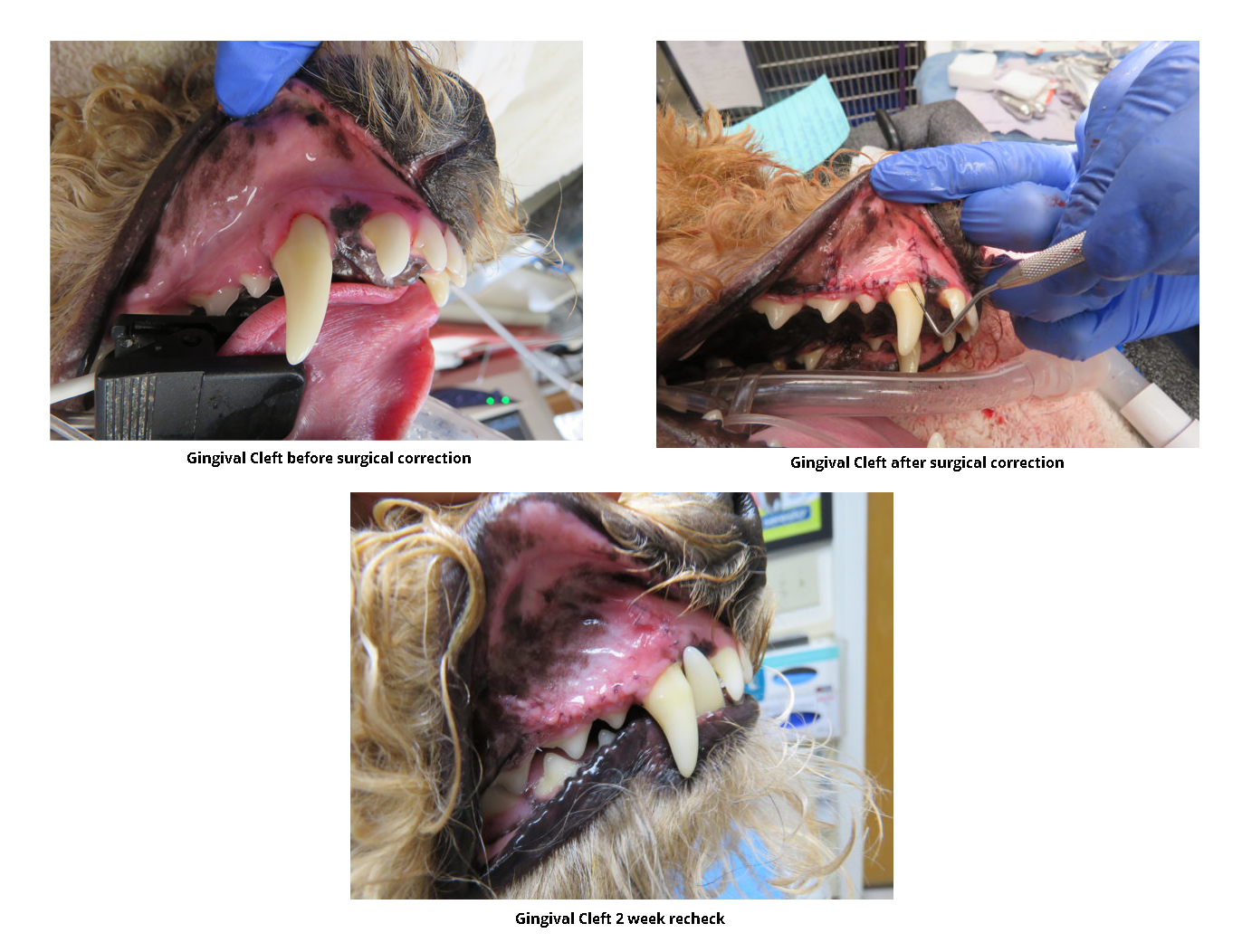
Treating Gingival Enlargement in Dogs and Cats
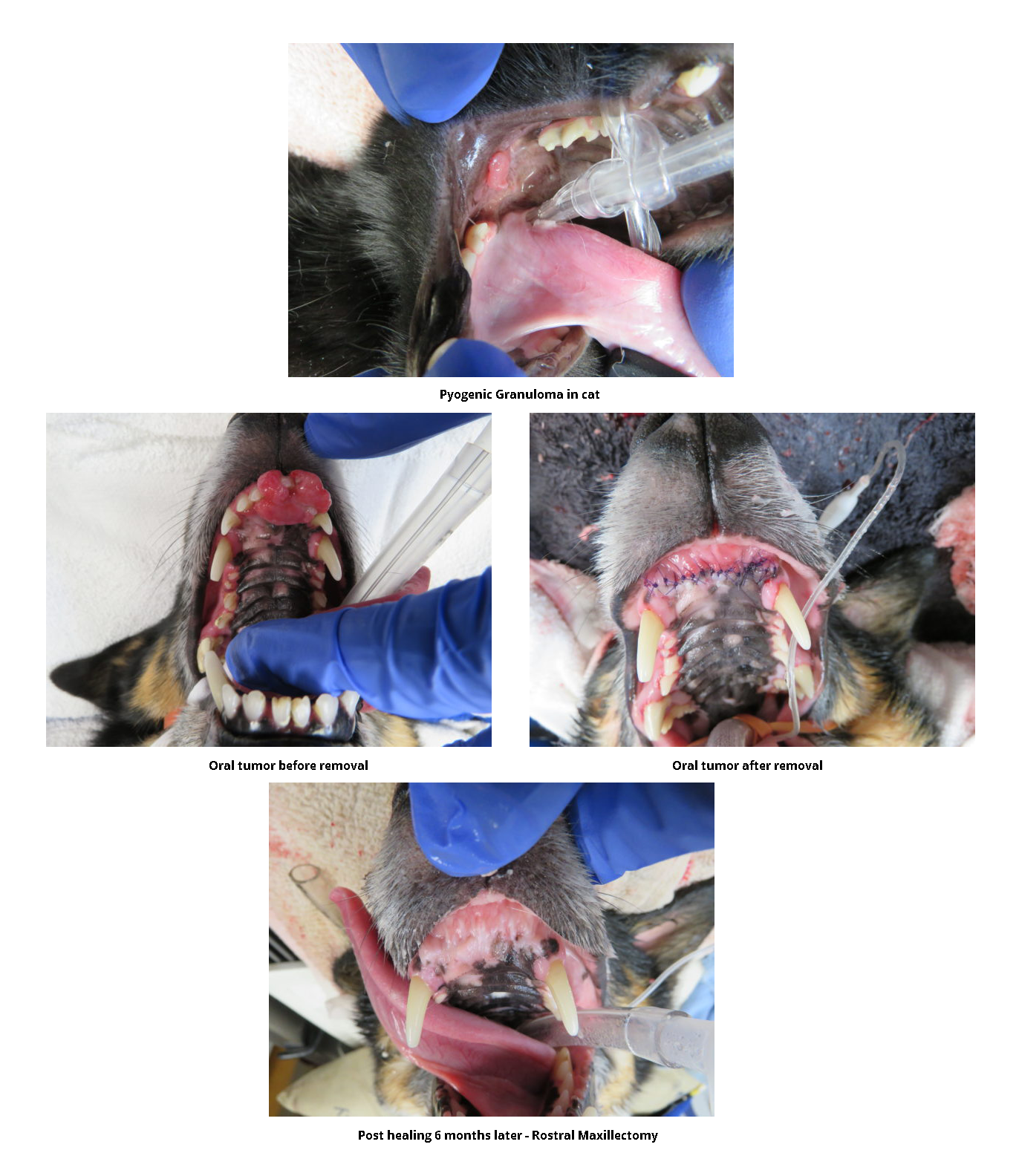
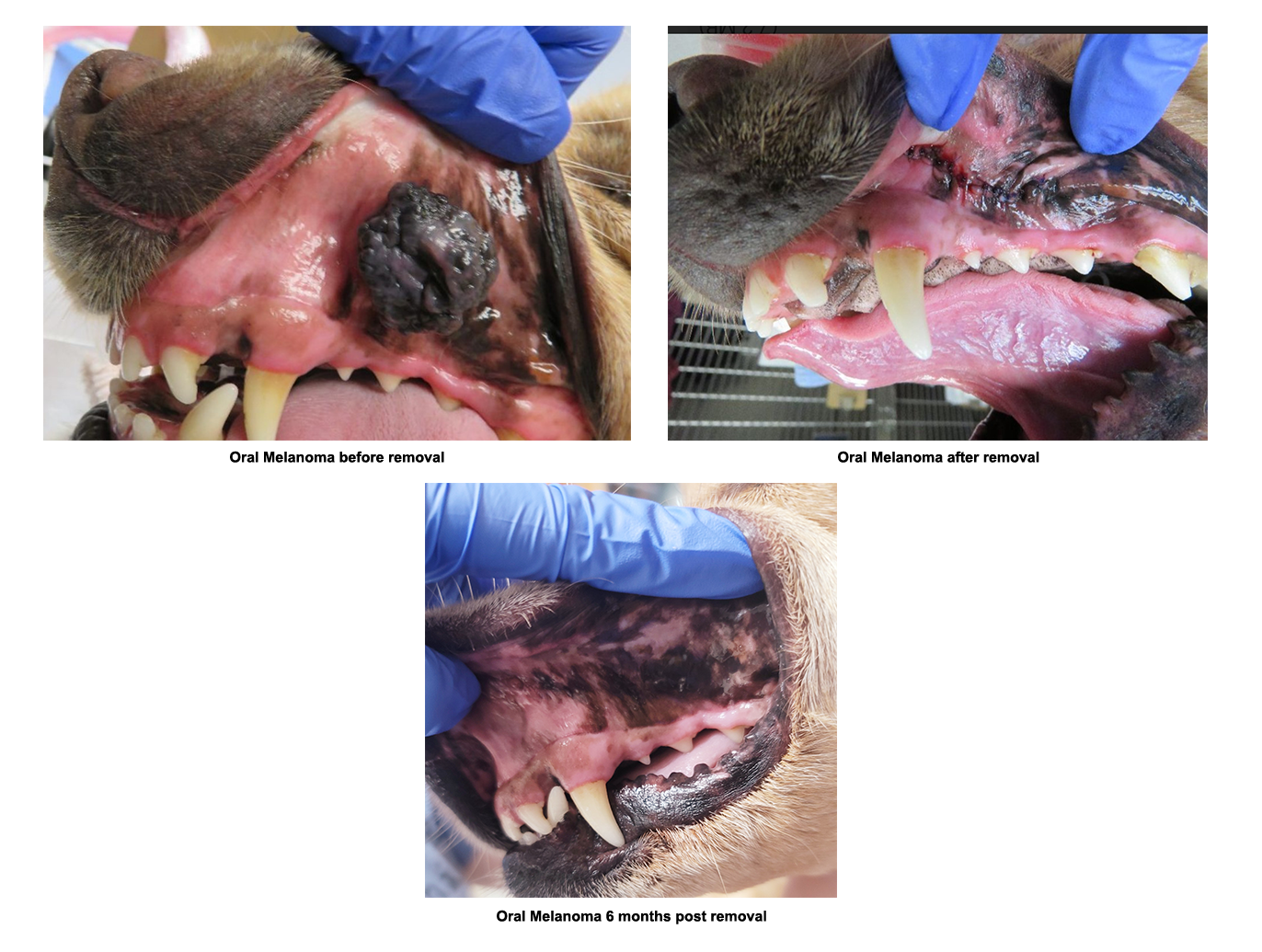
Pet Oral Tumors and Cancer
It is important to diagnose tumors as early as possible. Frequent inspection of the mouth is critical to monitor and detect changes or abnormalities. This can be done by daily tooth brushing to reduce plaque and calculus and aid in maintaining healthy gingiva.
Tumors can be either benign (non-cancerous) or malignant (cancerous). Benign oral tumors do not spread to other parts of the body; however, can be severely locally aggressive. Malignant oral tumors invade the surrounding tissue along with the potential to spread to other parts of the body, particularly local lymph nodes, lungs, or even distant organs. Not all oral tumors present as large growths, some start as non-healing wounds or ulcers.
Intraoral dental radiographs are essential to assess tumor characteristics, in particular the extent the tumor has or has not invaded the bone or surrounding tissue. A careful evaluation to determine the best approach for the patient begins with radiographs. Radiographs may also assist the clinician to determine if the tumor is benign or malignant, although histopathology will provide a clearer picture of the type of tumor and its clinically aggressive or non-aggressive nature. The best way to determine what type of tumor may be affecting your pet’s mouth is by obtaining a biopsy (taking a small portion of tissue that is examined under a microscope) that is reviewed by a boarded oral pathologist. Additional advanced imaging or diagnostics may be recommended to assist in staging. Staging is the ability to determine the extent of cancer, as well as if it has spread to nearby lymph nodes or other parts of the body. Advanced diagnostics, which may be recommended, are computed tomography (CT) to visualize the extent of the tumor as well as can assist with 3D rendering; lymph node aspirates can assist to determine if the tumor has spread to local draining lymph nodes, chest radiographs (x-ray of the lungs), and abdominal ultrasounds. Not all of these diagnostics are always recommended, but it is important to know that these tests may be vital in providing a clearer clinical picture of your pet’s condition and assist in determining the best course of action.
When it comes to tumors, it is important to not just “wait and see.” The tissue in the mouth heals fast and grows fast; therefore, this approach is not recommended and should be avoided. Palliative care may be a viable option to provide patients comfort during the end of their life. These options would be discussed with you to relieve your pet’s pain.
For most oral tumors that affect our patients, surgical removal often provides the best chance for a cure or better quality of life. After the surgery is performed, it may be recommended to seek further care with a referral to a veterinary oncologist. Early detection is the key to successful treatment with oral tumors.
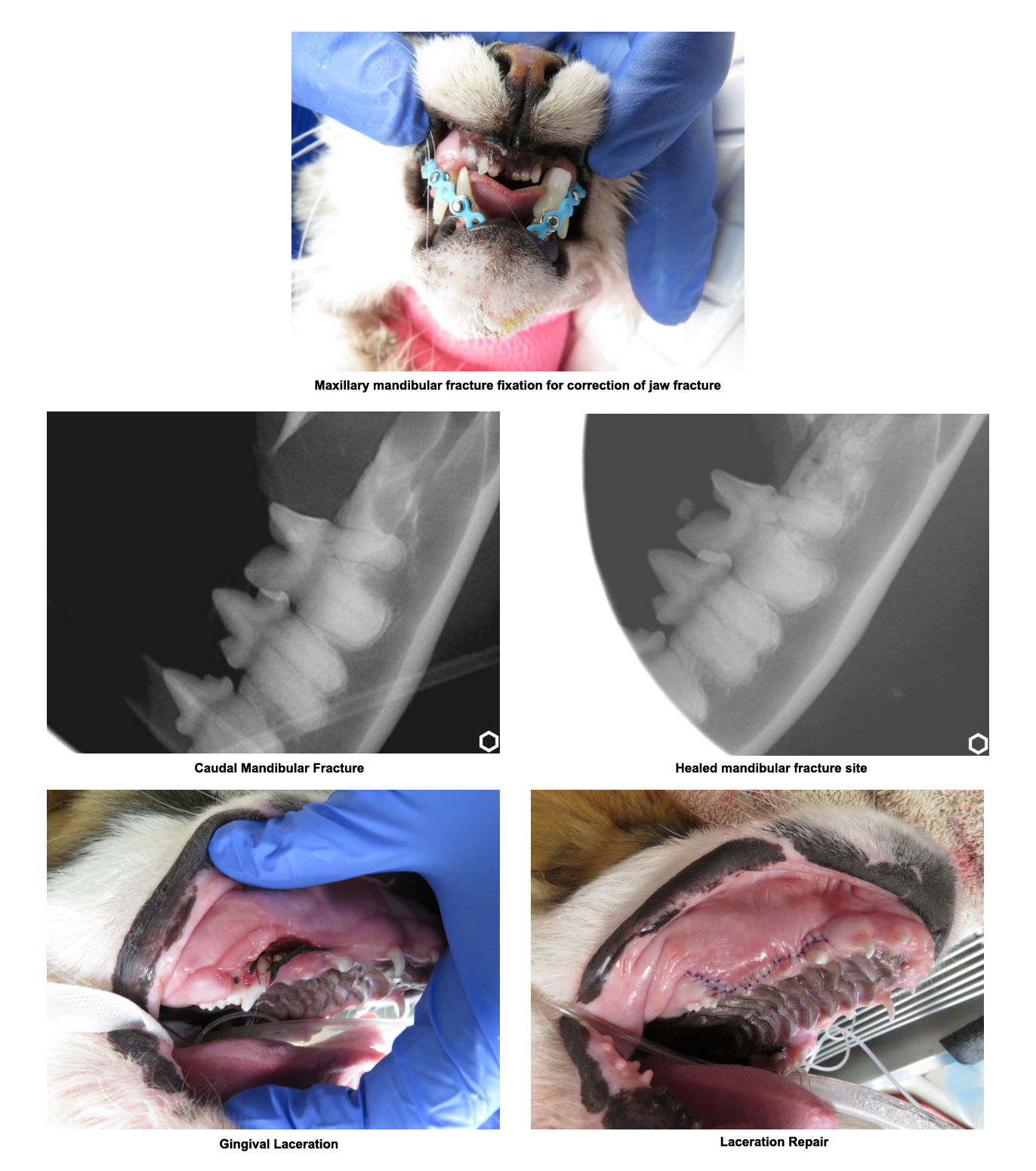
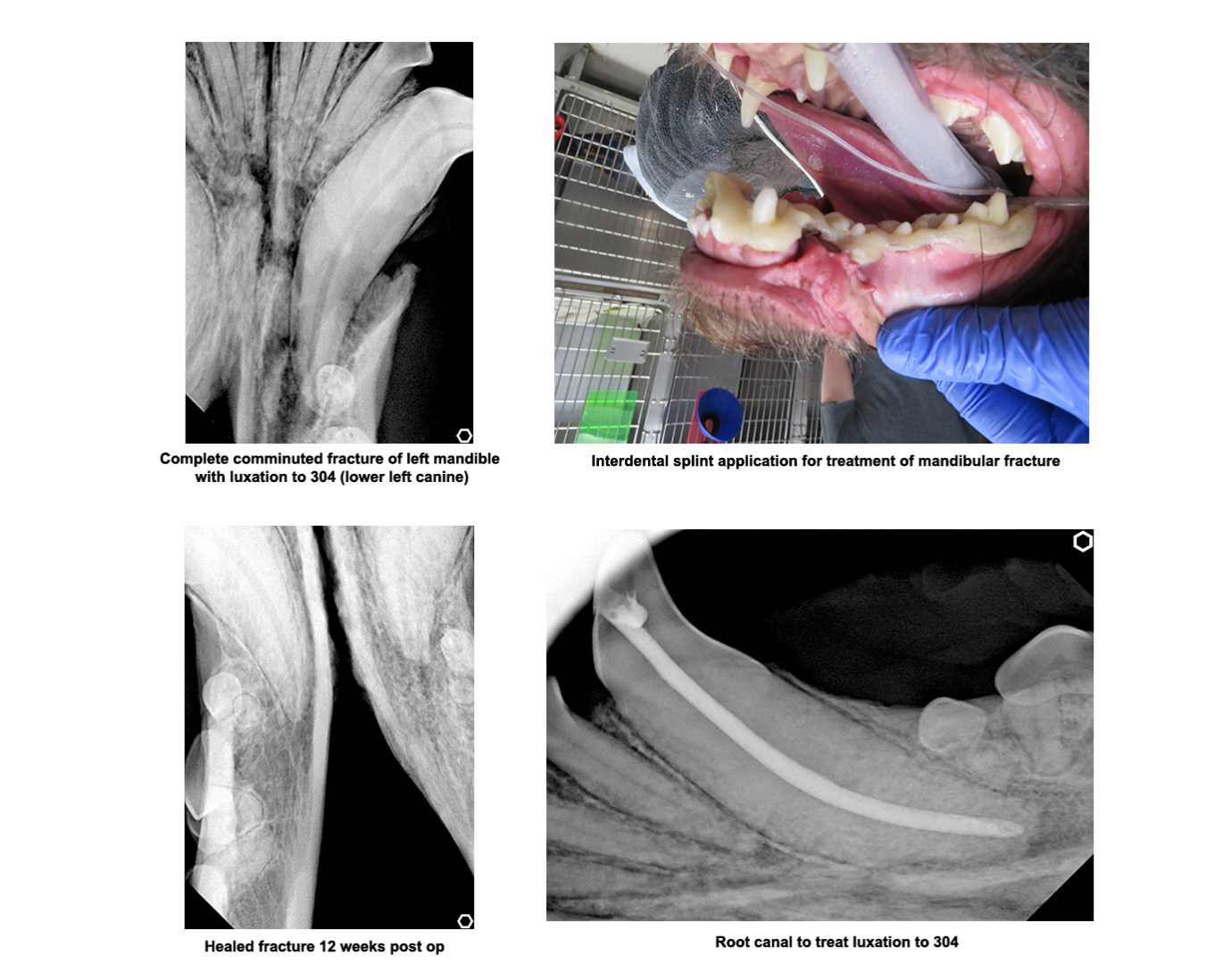
Jaw Fractures & Oral Trauma
The healing time may vary depending on the age of the patient as well as the severity of the fracture. Typically healing time occurs within 4 to 8 weeks. Older dogs may require a longer length of placement for splints/wire than younger dogs. Typically at a 2-week recheck, we will determine to follow-up care and when to remove the appliance (if one was used).
In severe jaw fractures or temporomandibular joint luxations (TMJ luxation) placement of an appliance to reduce motion is often necessary to allow for healing. This can be accomplished with a soft muzzle, maxillary mandibular fracture fixation devices or usage of buttons (such as the labial button technique). These options will be provided based on the pet’s type of fracture or luxation and available techniques to promote appropriate healing. The goal of any treatment is a comfortable occlusion and a mouth free of pain and infection.
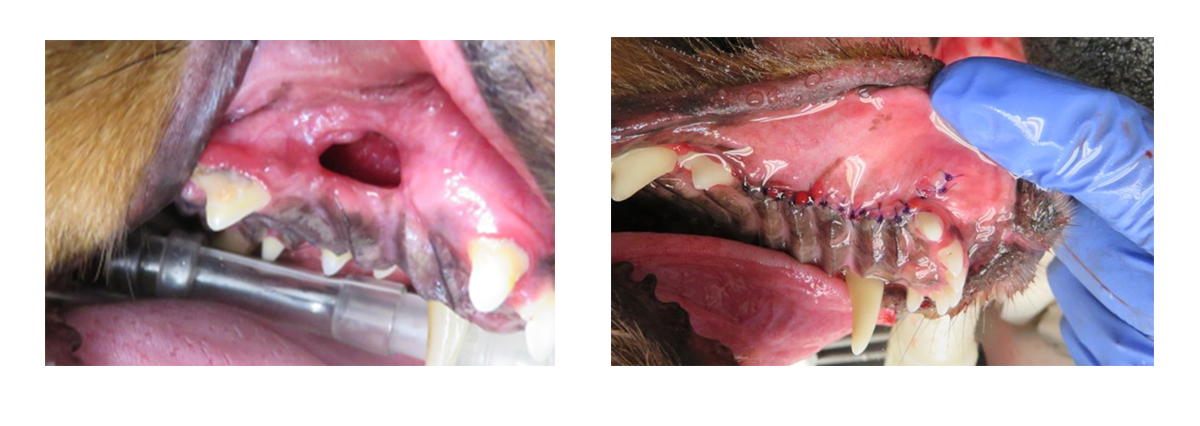
Oronasal Fistulas
Oronasal fistulas can occur in pets. Common causes of fistula formation include periodontal disease, an overly aggressive extraction of a pet’s tooth, incomplete healing after tooth extraction, or due to malocclusions where the lower canines are causing trauma to the roof of the mouth.
Dachshunds, in particular, are predisposed to periodontal disease, and one of the main locations where they can have bone loss is on the palatal aspect (roof of the mouth) of the maxillary canine teeth (upper canine). There is a very thin shelf of bone between the canine tooth and the nasal cavity. When there is bone loss in this area, it can lead to an oral-nasal fistula (abnormal communication between the nose and the mouth). If there is an oral-nasal fistula present, food/water/debris can become entrapped in this area and cause chronic irritation to the nasal cavity, leading to nasal discharge and sneezing.
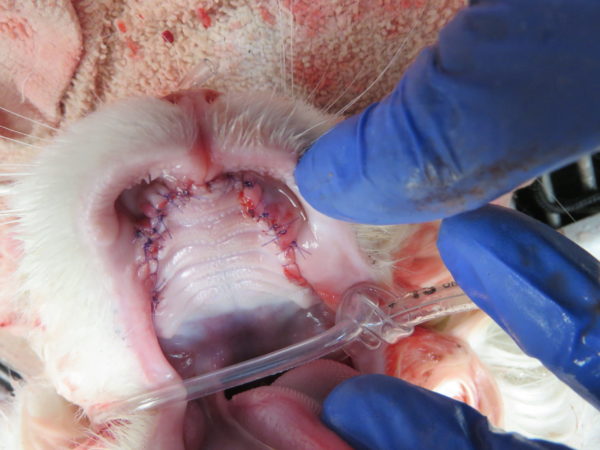
Treatment is required for this condition and the best success is having this treated in a single procedure with a single mucogingival flap (an area of tissue inside the mouth) that has absolutely no tension. For chronic or severe oronasal fistulas they may require a double-layer flap technique.
After the surgery is performed for treatment of an oronasal fistula, they typically are sent home with antibiotics and pain medications. Clients are often instructed to feed soft food for a minimum of 14 days and potentially longer depending on the severity. Patients will always require an examination 2 weeks following surgery to ensure the area is healing and educate when the pet can start back on hard food and toys.
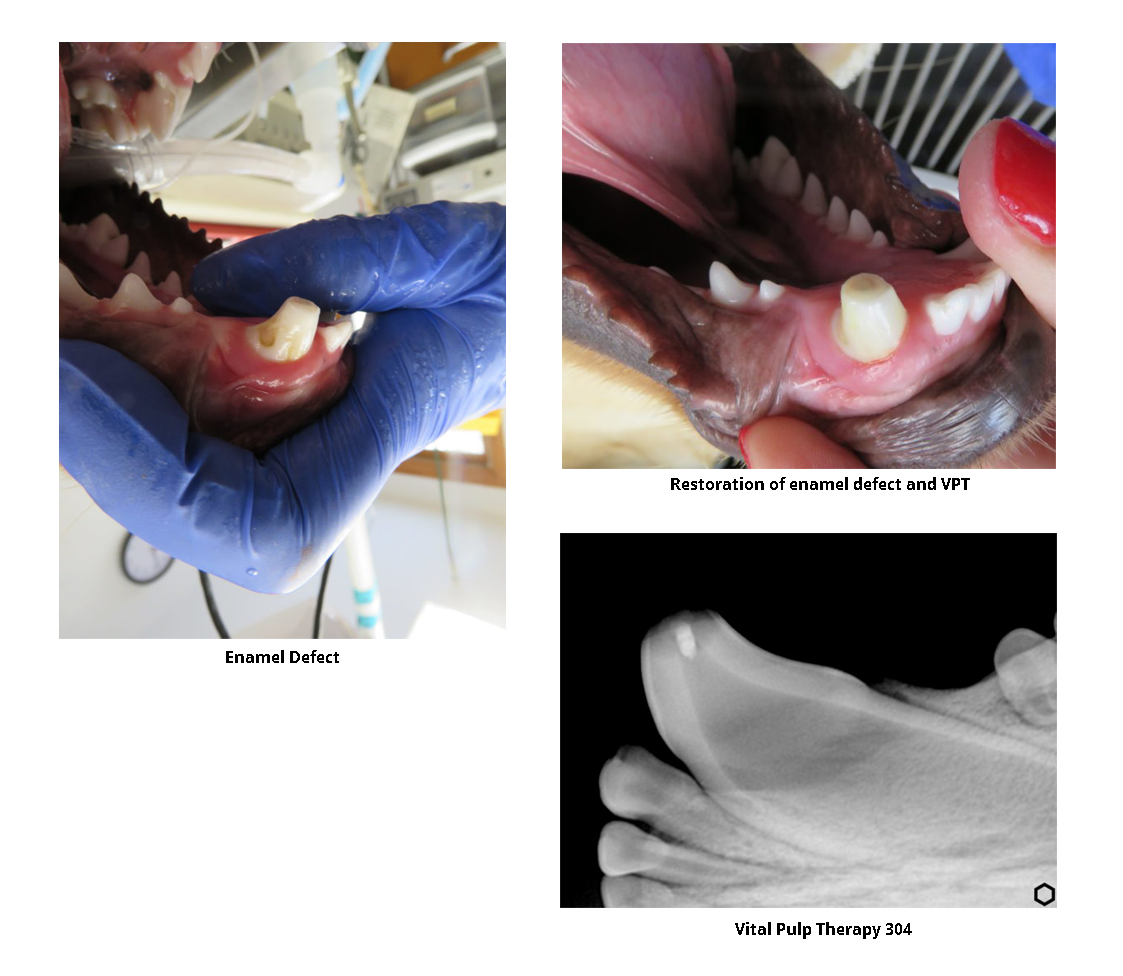
What does a discolored tooth mean for your pet?
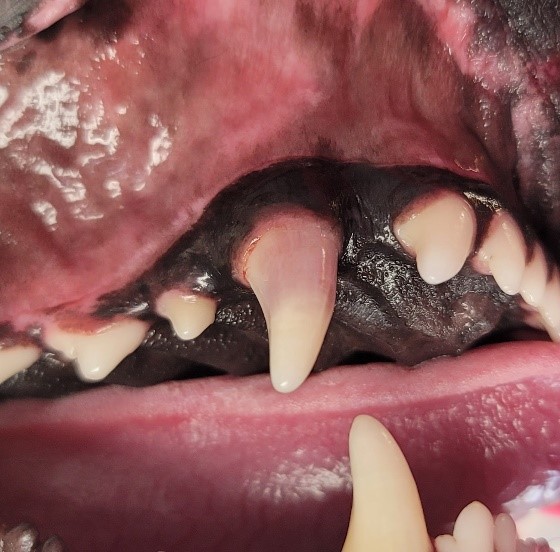 It has been published recently that 87.6% of discolored teeth are histologically non-vital (i.e. dead). A previous study prior to this which did not include pathology found 92.2% of discolored teeth non-vital. Therefore, with the knowledge from these important papers it is therefore recommended that discolored teeth should not be ignored.
It has been published recently that 87.6% of discolored teeth are histologically non-vital (i.e. dead). A previous study prior to this which did not include pathology found 92.2% of discolored teeth non-vital. Therefore, with the knowledge from these important papers it is therefore recommended that discolored teeth should not be ignored.
What makes up a tooth?
There are 3 important structures which make up the tooth which are:
- Enamel (external substance and the hardest in the body)
- Dentin (porous like coral which takes up the majority of the tooth)
- Root canal (i.e. the pulp) which contains the vein, artery, and nerve.
The pulp is what provides the tooth vitality (i.e. the tooth is alive). The pulp cannot expand because it is encased in the center of the tooth; surrounded by the hard tissues of the tooth which are described above.
How does a tooth discoloration occur?
Discolored teeth often occur due to concussive injury. When the blood supply is compromised due to the swelling of the pulp. This is called irreversible pulpitis. Most of the time, if not all the time, the tooth dies. When the tooth appears discolored it can vary between pink to purple-gray. Like a bruise on the skin, the color change is a result of hemorrhage (i.e. bleeding) within the tooth.
Is a discolored tooth painful?
Initially when the pulp suffers injury it is extremely painful (we know this by asking people who have had this condition) then after the pulp dies it is not painful. After time, it often becomes painful again when the tooth becomes infected (i.e. abscessation).
How does a veterinarian diagnosis a non-vital tooth?
Usually, pulpitis can be determined visually. If the tooth appears intrinsically discolored (a color change from within, not on the exterior), then pulpitis has occurred. In addition to a complete oral examination, dental x-rays may be obtained to help assess the tooth status. Unfortunately, in 42% of discolored teeth, x-rays appear normal, as it often takes time to see a change on x-ray. Likewise, humans experiencing discomfort due to pulpitis do not always show changes on x-rays. In people they will often do thermal testing where they either apply either increased or decreased temperatures to stimulate the pulp sensory response. These types of tests are unreliable in our patients as our patients cannot speak to indicate if it hurts. We use the combination of dental radiographs, oral exam, and publications to make the appropriate recommendation for your pets’ tooth issue.
Some may ask why to treat a discolored tooth?
Dogs and cats are very stoic and often mask pain. We know from people this condition is incredibly painful! This is especially true in the early and late stages of the process. Through a process called anachoresis, bacteria naturally found in the bloodstream may be attracted to the area of the dead pulp and set up a thriving community. The active bacterial population leads to more inflammation as well as pain and can possibly spread to the body.
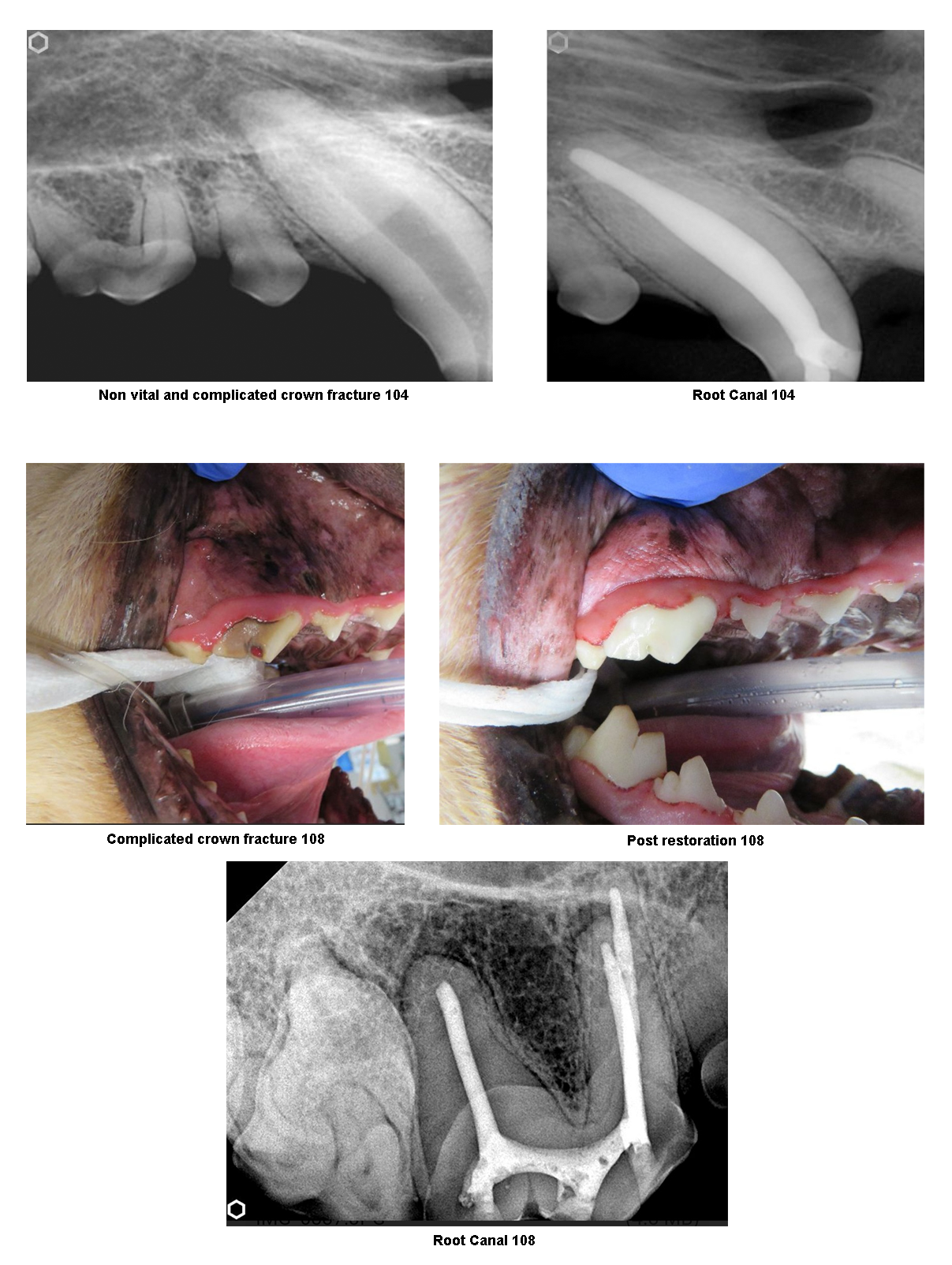
What are the treatment options if my pet has a discolored tooth?
If the staining is only on the surface, the discolored dog or cat tooth may not require treatment. However, discolored teeth that are dead or painful are treated with endodontic (root canal) therapy or extraction. Depending on the severity of the problem and the type of tooth affected a recommendation of one of these two treatments may be made.
- Endodontic therapy is also known as root canal therapy. This treatment involves removing the dead pulp within the tooth, cleaning and disinfecting the hollow area inside the tooth, and filling the inside of the tooth with materials that prevent any re-entry of bacteria inside the tooth. Root canal therapy is a less traumatic procedure than extraction and allows the tooth to remain in your dog or cat’s mouth. See more about endodontics therapy at Lake County Veterinary Clinics, by clicking the link below.
- Surgical extractions are recommended in severe cases where a root canal is not an option. Surgical extractions are more invasive than root canal therapy, as the roots of a dog or cat’s teeth go deep into the jawbone. Teeth are like an iceberg as the majority of the tooth lives below the gumline. Unfortunately, sometimes surgery is the only available option.
Endodontics (Root Canal Therapy)
When possible for specific strategic teeth, we recommend endodontic therapy (aka root canals). This is to allow our patients to have a functional mouth free of pain and discomfort. The goal of Root Canal Therapy is to carefully debride and disinfect the pulp chamber and root canal system of the affected tooth, and then seal it with material that will prevent future internal infection of the endodontic system of the tooth from recurring. The peri-apical pathology that develops from endodontic infections will be expected to self-resolve once the chronic source of infection from inside the tooth is eliminated. Radiographic evidence of healing should be evident in approximately 6 months but may take longer to completely heal. In some cases, the procedure is not successful and additional surgical care may be indicated. If you have questions if your pet is a candidate for this procedure, ask our doctor team.
Periodontics
Periodontal disease is one of the most common diseases in our canine and feline friends. Periodontal disease begins when bacteria form a substance called plaque which sticks to the surface of the teeth. Once the plaque is present, minerals in the saliva harden the plaque into dental calculus in about 24-48 hours and is firmly attached to the teeth. Problems develop as plaque and calculus spread under the gum line and bacteria in the plaque causes damage to the supporting tissues around the tooth. This eventually leads to loss of the tooth. Bacteria under the gum line secrete toxins which contribute to tissue and bone loss. This stimulates the animal’s immune system and furthers the local inflammation. Periodontal disease includes gingivitis (inflammation of the gums) and periodontitis (loss of bone and soft tissue around the teeth). A strict oral care regimen at home will hopefully delay the progression of this condition in your pets’ remaining teeth. Here at Lake County Veterinary Clinics, PLLC we recommend a comprehensive dental exam and treatment plan with prophylaxis (dental cleaning) once a year to ensure a healthy mouth for years to come.
Crowns & Restoratives
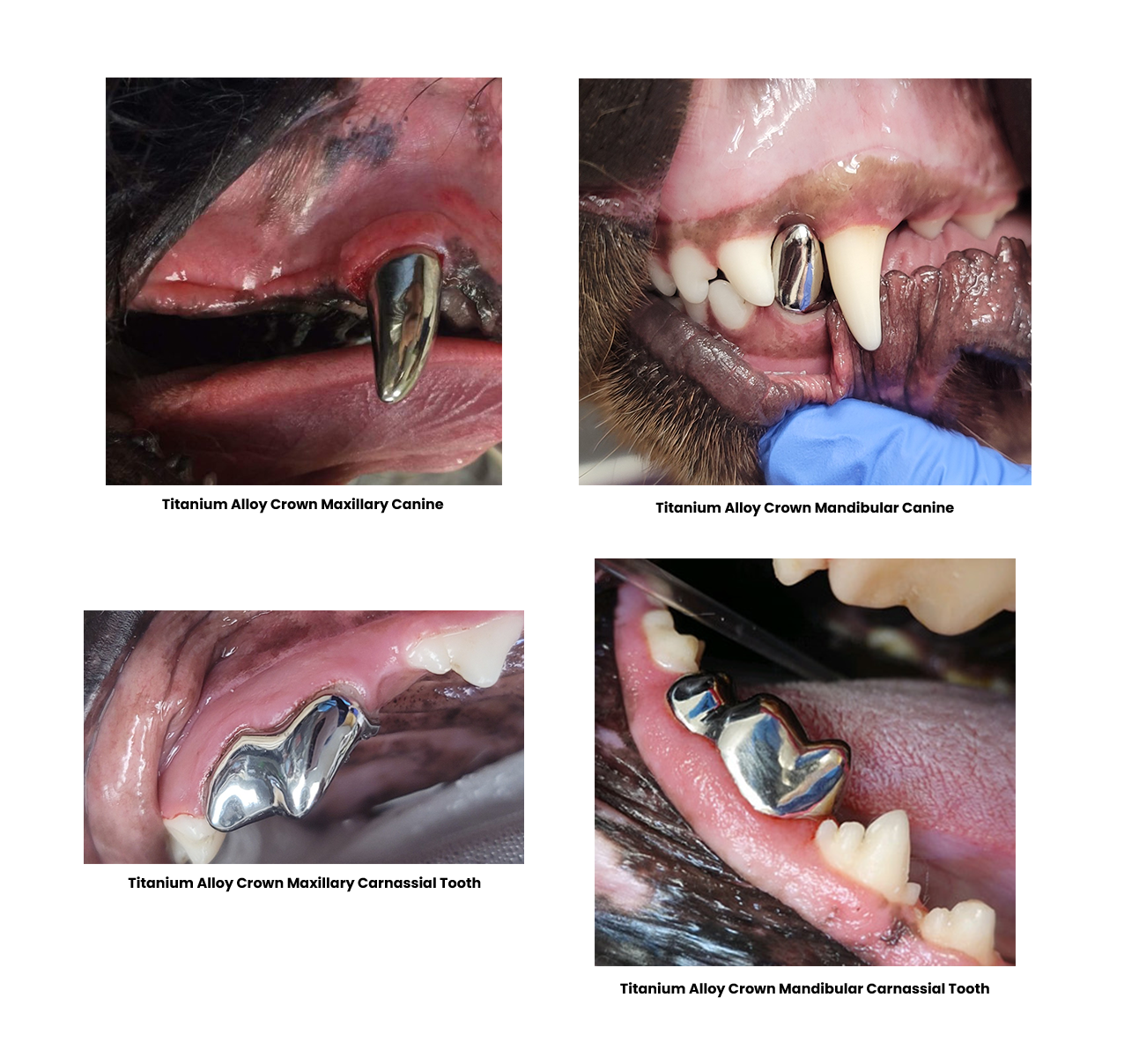
Crowns
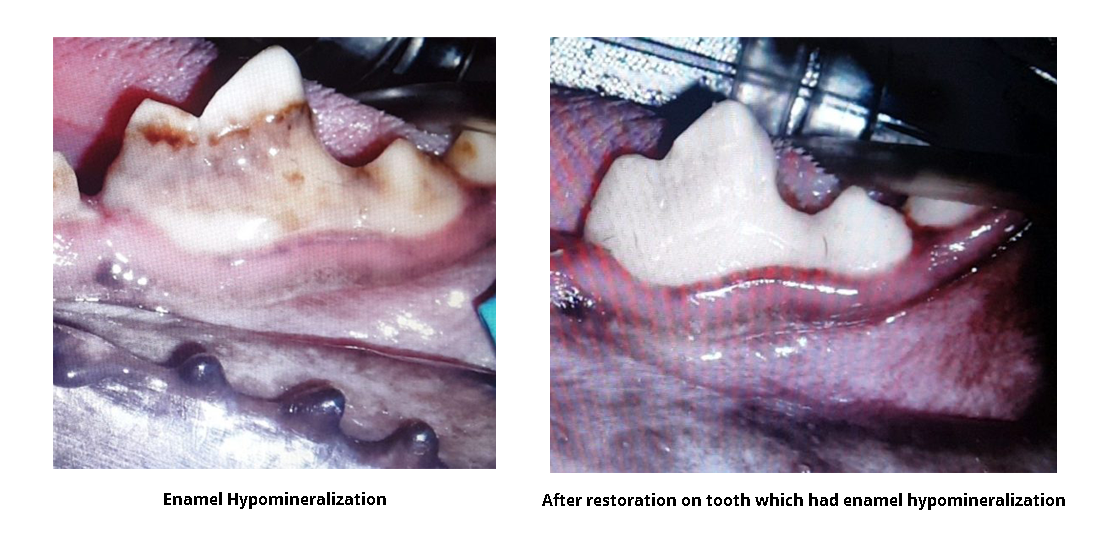
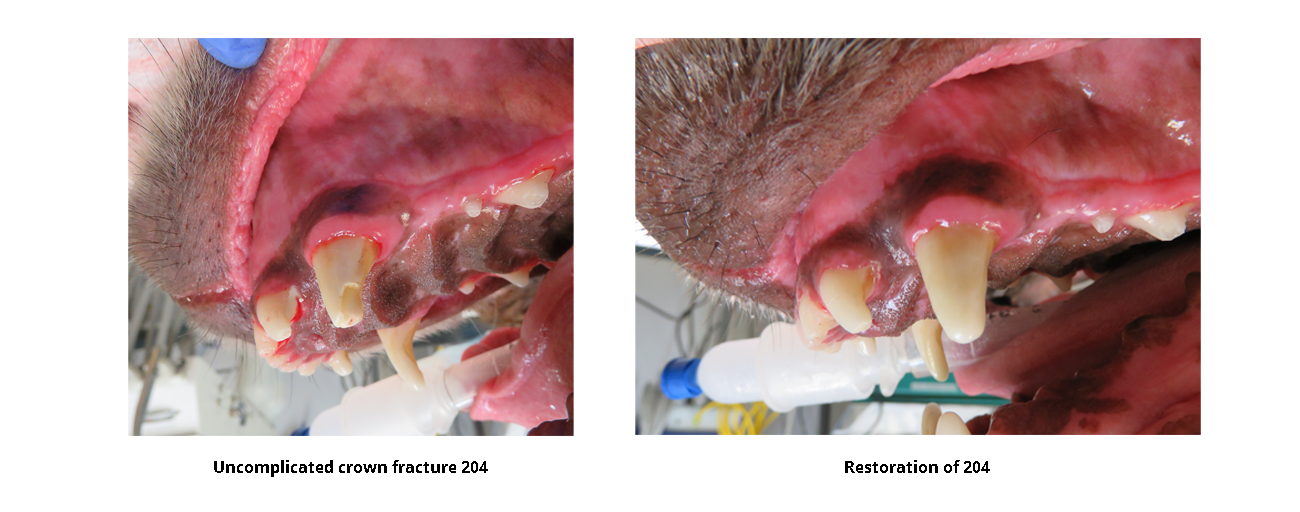
Restoratives
Orthodontics
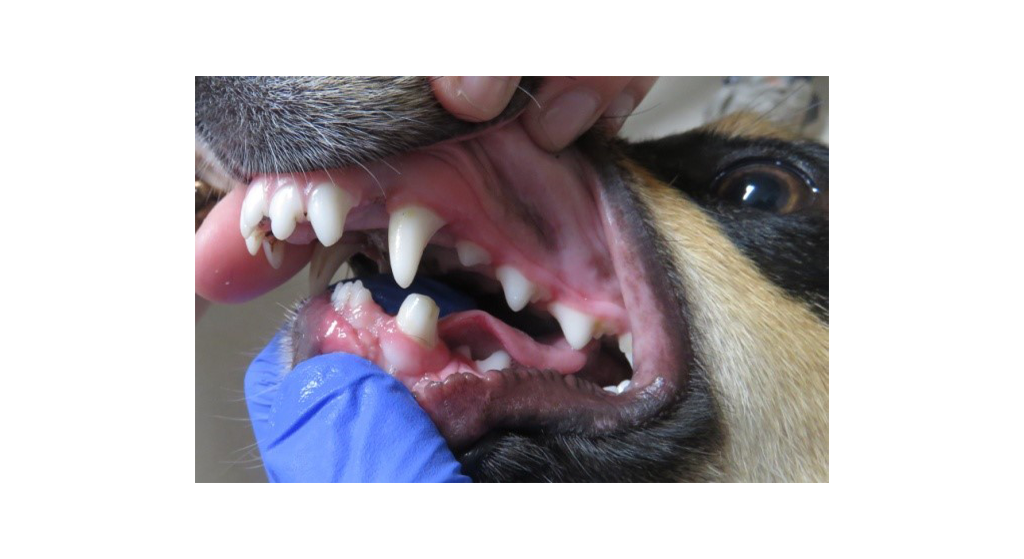
- Orthodontics is typically recommended for patients who have malocclusions. Malocclusions are misalignment of the normal jaw. Typical jaw alignment is a “Class 0” or normal occlusion (a normal scissor bite). The “scissors bite” refers to the normal relationship between the upper and lower teeth. For a true “scissor bite,” the upper incisors overlap the lower incisors when the mouth is closed. The lower canine teeth fit in between the upper third incisor and the upper canine without touching either of them with the mouth closed. In viewing the teeth from the side with the mouth closed, the premolar teeth of the upper and lower dental arcades interdigitate very much like the teeth of “sheer scissors”.
- For patients who have true malocclusions, they may be a candidate for orthodontics. This is a procedure which can allow the normal permanent dentition to come into appropriate alignment which reduces oral discomfort in the future.
- Types of orthodontic procedures we can do at Lake County Veterinary Clinics, PLLC
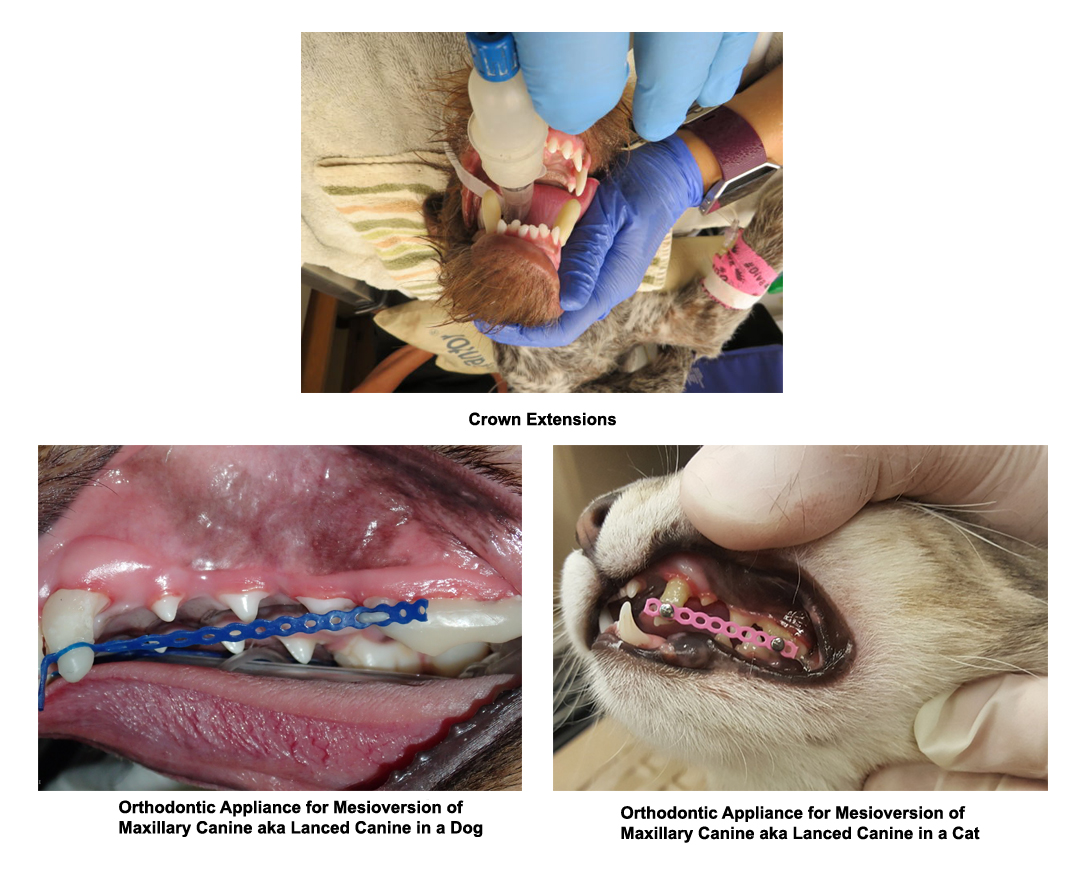
- Crown Extensions (application of composite placed on lower canines to correct lingoversion mandibular canines).
- Arch Bar (appliance placed on maxillary “upper” incisors and canines to correct underbite.
- Correction of mesioversion to maxillary canine (lanced canine) via orthodontic appliance.
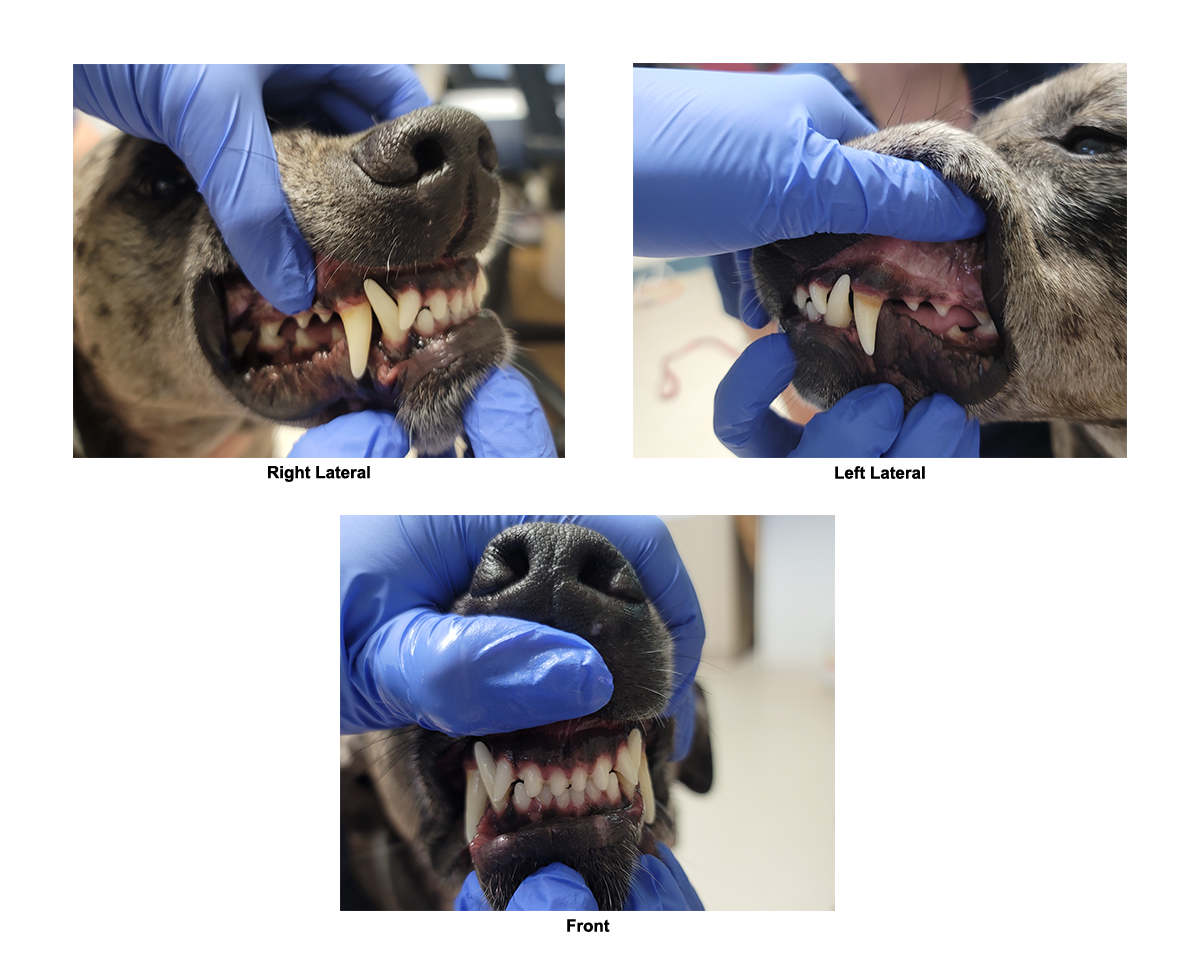
Malocclusion
Normal occlusion – Class 0
- The normal occlusion is a scissor bite. This is where the mandibular (lower canines) interdigitate with the maxillary (upper) canine and lateral maxillary (upper) incisor teeth. The maxillary (upper) incisors should be in front (rostral) of the lower incisors.
Malocclusion – a deviation from normal occlusion
- A malocclusion is an abnormal alignment of the teeth, also called an abnormal bite.
- This could be related to malpositioned dentition or skeletal changes which create one jaw to be longer or shorter to the other.
- Malocclusions can be harmless (such as normal breed abnormalities like underbite), or they can be a problem for your pet when there is abnormal tooth-to-tooth or tooth-to-soft tissue contact.
- This tooth-tooth or tooth-soft tissue contact can cause pain and long-lasting side effects that have a negative impact on your pet’s health unless the malocclusion is addressed.
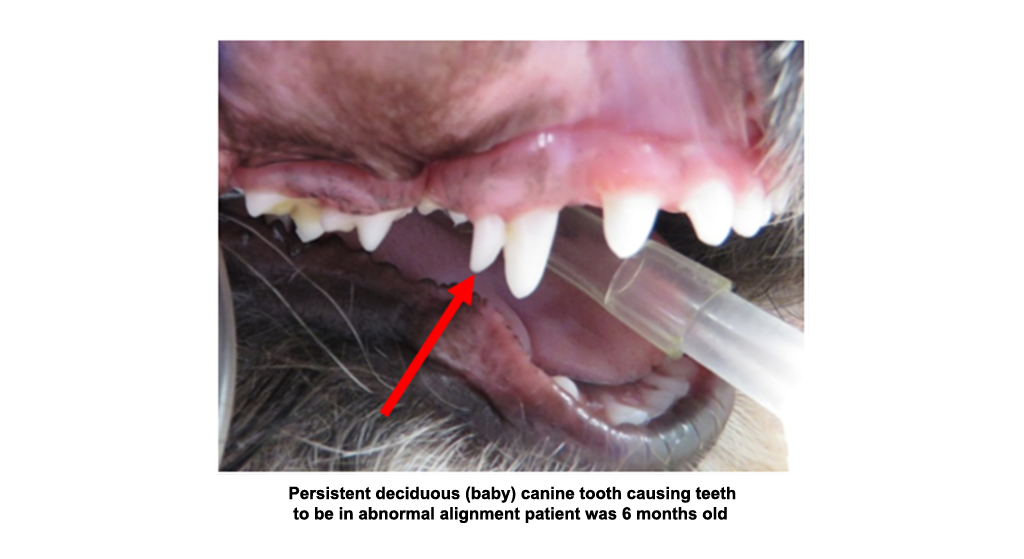
- A malocclusion can involve one or many teeth and can be due to genetic causes, trauma, tumors or infections that cause teeth to erupt abnormally. Baby teeth that fail to fall out can cause malocclusions to develop.
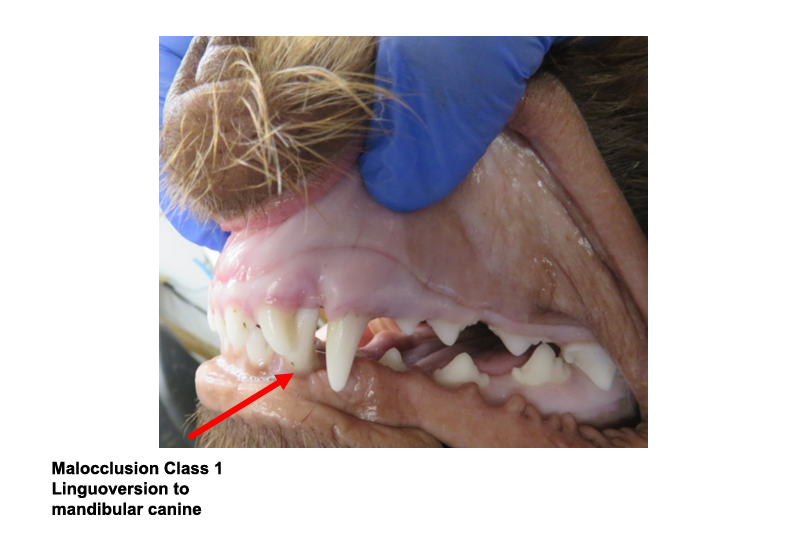
Class 1 malocclusion – normal jaw length and shape, however one tooth is out of alignment (see orthodontic page for additional information)
- Example: linguoversion to mandibular (lower) canine (also known as based narrow canine) is where the jaw is normal length but the lower canine is fixed more inward (palatal) and upright and towards the inside of the mouth (lingual).
- This can be caused by persistent deciduous (baby) teeth which prevent the tooth from erupting normally. Trauma can occur to the upper jaw if not corrected. There are several treatment options for this condition.
- In puppies, performing extraction of deciduous teeth is imperative to relieve the trauma to allow the lower jaw to continue to grow. This procedure is known as interceptive orthodontics.
- In late puppies to adult teeth, other options are ball therapy, crown extensions, gingivectomy with or without crown extensions, incline plane, crown reduction with vital pulp therapy, or extractions of mandibular (lower) canines.
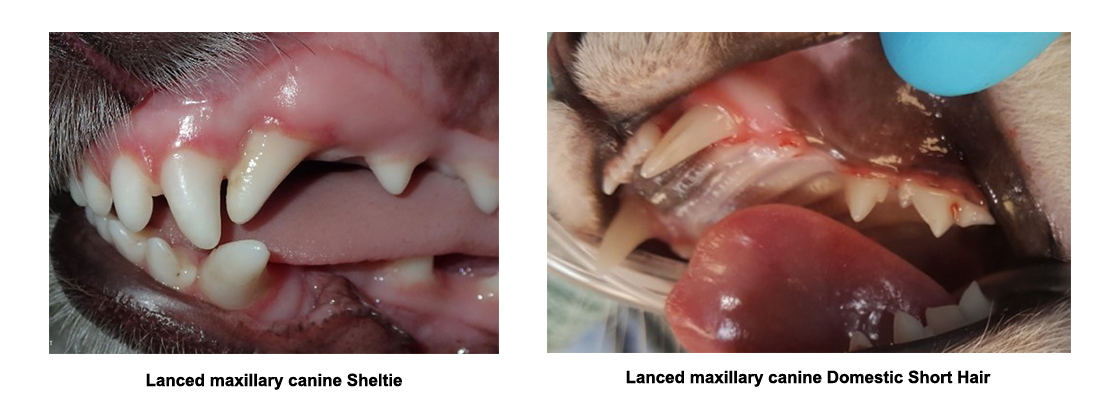
- Example: mesioversion to maxillary (upper) canine (also known as lanced canine) where the tooth is located in the (mesial) direction more forward.
Class 2 malocclusion – occurs when the upper jaw is longer than the lower jaw (see orthodontic page for additional information)
- This is a genetic skeletal deformity. The short jaw can cause the mandibular canine teeth or incisors to traumatize the palate and gum tissue of the upper jaw which can lead to damage and pain.
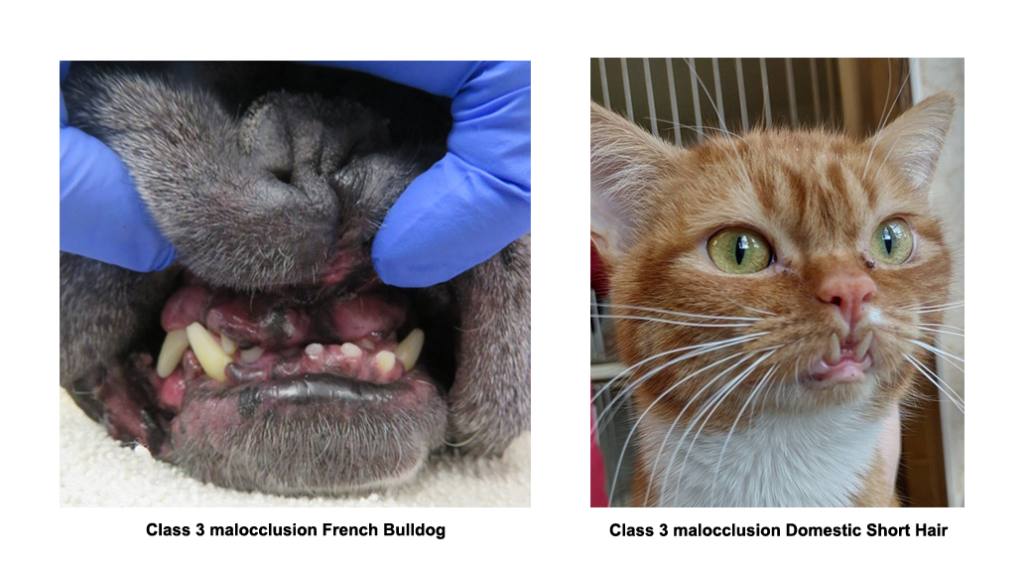
Class 3 malocclusion – occurs when the lower jaw is too long relative to the upper jaw and the lower teeth protrude in front of corresponding upper teeth known commonly as an underbite.
- This genetic skeletal condition may be normal for some breeds such as French bulldogs, boxers; however, it can cause abnormal contact to maxillary (upper incisors) making abnormal contact and cause damage to teeth and gums. The short maxilla (upper jaw) can also result in crowding and rotated teeth which can cause abnormal wear leading to a rapid onset of periodontal disease.
Class 4 malocclusion – is known commonly as a wry bite of the jaws, clinically as Maxillomandibular Asymmetry. This is where one part of the jaw is longer than the other part.
- This leads to left-to-right asymmetry of the jaws, meaning that they may have an “open bite” where their teeth cannot fit together normally and the upper jaw may look as though it is to one side or the other of the bottom jaw. This usually is caused by trauma when the jaws are growing and leads to different growth rates to each jaw part.
Management of Malocclusion:
- Orthodontics: This is a specialty in dentistry and oral surgery concerned with prevention and correction of malocclusion to alleviate trauma to the mouth. Mouths of animals do not have to be aesthetically pleasing however they should be free of discomfort.
Preventative Orthodontics:
- This is a preventative procedure which is undertaken in anticipation of a developmental problem.
- Examples:
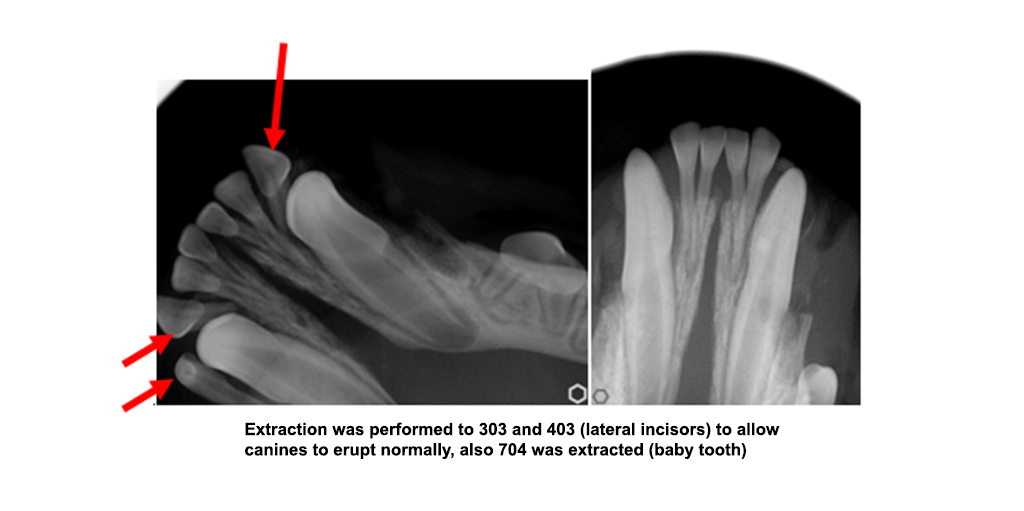
- Interceptive orthodontics: removal of a tooth to reduce trauma to permanent dentition or to allow for a normal path for an adult tooth to erupt normally.
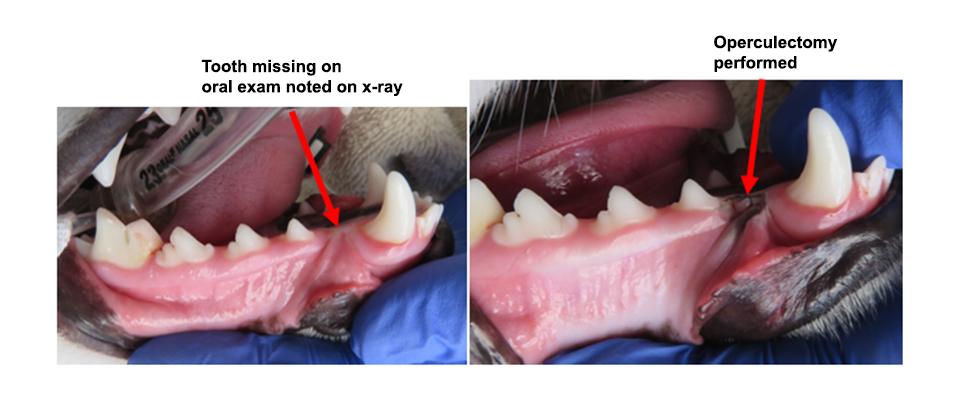
- Operculectomy: removing gingival tissue (or sometimes bone) that is above the impacted tooth, which could inhibit the tooth from erupting leading to cystic formation in the future if the tooth does not erupt.
Causes of Malocclusions:
- Retained primary (deciduous) teeth: If a baby tooth fails to fall out, and is still present as the adult tooth erupts, a malocclusion will likely develop. This is probably the most common cause of malocclusions in dogs and cats.
- Primary teeth should shed before the permanent teeth erupt.
- The primary teeth cause abnormal crowding, forcing the permanent teeth into abnormal position. It is especially important to monitor permanent tooth eruption from age 4-7 months.
- “No two teeth should occupy the same space at the same time!”
- Genetics, Abnormal Growth: typically result in class II or III malocclusion, where one jaw is shorter than the other jaw, most often due to a hereditary genetic trait.
- These dogs and cats should not be bred and the breeder should be informed of the problem so they can avoid breeding the parents of the dog or cat in the future.
- Trauma: Occasionally, we see dogs or cats that had some form of head trauma when they were still growing. This can lead to a malocclusion if the jaw growth is misaligned, or if an individual tooth is damaged and erupts in a different position than normal.
- Linguoverted or Base-Narrow Mandibular Canine teeth: The most common form of malocclusion in dogs is where the lower canine teeth are traumatizing the upper jaw.
- See orthodontic page for more information
- Mesioversion to maxillary (Lanced) canines: the maxillary (upper) canine teeth sometimes erupt horizontally, causing the tip of the crown to point forward rather than down. This is most commonly seen as a genetic defect in Shetland sheepdogs, Italian greyhounds, Fox terriers and miniature Schnauzers, though it can occur in any breed as a result of a persistent baby tooth.
- See orthodontic page for more information
**An important note about orthodontic correction. ** Movement of teeth is a procedure that requires proper materials and a degree of expertise in dentistry. Improperly applied orthodontic devices can cause more harm than benefit and permanently damage the teeth and gums. Orthodontic correction should never be undertaken without a thorough bite evaluation and an understanding of the type of tooth movement and appliance needed. In addition, it is unethical to show a dog after orthodontics has been performed to correct a genetic malocclusion. If you have any questions, please feel free to discuss these with us at your consultation.
Feline Dental Disease
Feline Stomatitis
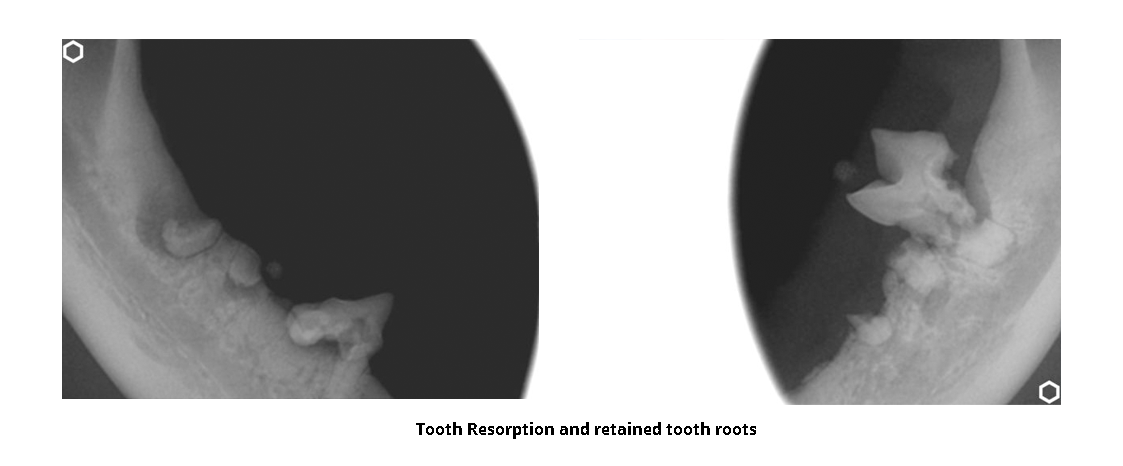
- Stomatitis is a chronic, wide-spread inflammatory disease affecting the gingiva and mucosal lining of any of the structures in the oral cavity. We think the cause is multifactorial and the inciting factor is likely an abnormal response to plaque. If tooth resorption, another common dental abnormality seen in cats, was also noted during your cat’s oral exam, it was likely triggered by the stomatitis. The treatment of choice for stomatitis is surgical correction by removal of the plaque retaining surfaces (i.e., the teeth). This involves surgical extraction of affected teeth and intraoral radiographs (x-rays) of the whole oral cavity to look for any retained roots that need to be extracted.
- The prognosis for full mouth extractions as a treatment for stomatitis is good in the majority of patients. Many patients show improvement at the two weeks recheck and those who do not need any more medications past that mark. 60% of patients resolve without need for further medical management, 20% of cats with subclinical stomatitis do not require additional medication, 13% do not respond initially, but respond with additional medical management (corticosteroids and analgesics), and 7% fail to respond to any treatment. The healing process from stomatitis takes some time, and your pet may not show the full extent of improvement from surgical treatment for as long as 6-8 months.
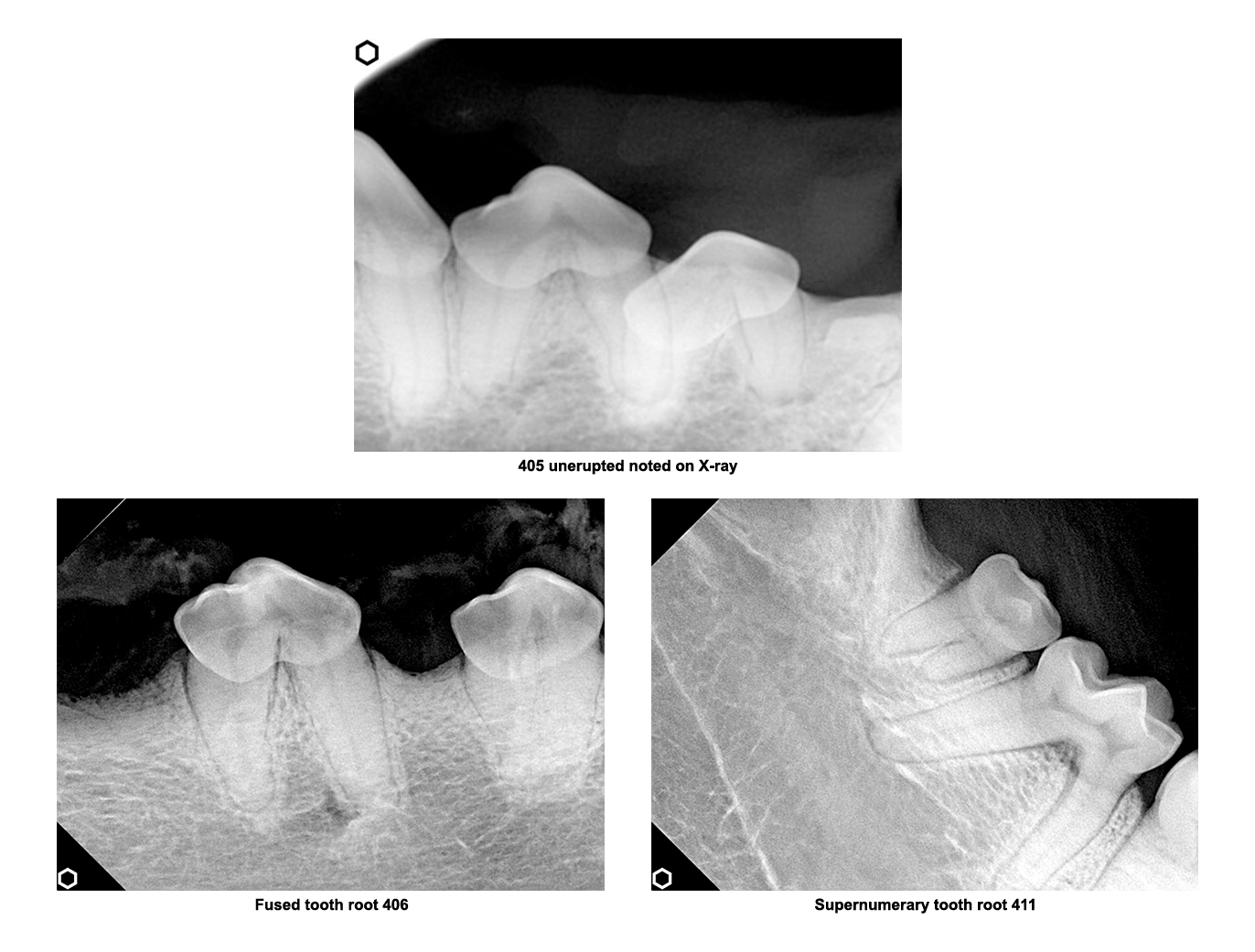
Intraoral Dental Radiographs
Intraoral dental radiology, or x-ray, is vital and essential for diagnosis, treatment, planning, and follow-up evaluation. Without quality radiographs, treating your pet’s oral issues would only be done with guessing. Dental radiographs are the standard and starting point for all oral care.
Anesthesia
Fear of general anesthesia for pets is a natural concern voiced by many owners when a veterinary dental procedure is recommended. However, the risk of chronic oral infection to your dog or cat, is far greater than the risk of an anesthetic complication. Some points to keep in mind when thinking about pet anesthesia are:
- When we go to our own human dentist or hygienist yearly or every 6 months we can sit quietly, open our mouth when asked, spit out water when requested and let the hygienist do their work. Our animal friends are not capable of remaining still, calm, and compliant during a dental cleaning without general anesthesia. While the principles of good oral hygiene are the same for dogs and cats as for people, there are some significant differences. Humans understand why the procedure is important, and we typically do not need sedation or restraint, but our pet’s do. To ensure that nothing is missed in dogs or cats, our patients require a thorough oral examination that includes digital dental radiographs, cleaning, and polishing under general anesthesia as part of a professional dental cleaning. We do this because “Fluffy” the cat will not allow the x-ray equipment in her mouth without sedation. “Bart” the 80-pound lab won’t sit still for cleaning without sedation. To provide the safest and most efficient care for both your pet and clinic staff these are services provided under general anesthesia.
- Anesthesia is essential for dental procedures, to ensure that the procedure can be completed successfully.
- Appropriately administered general anesthesia entails extremely low risk for the pet patient, as a result of a combination of pre-anesthetic assessment of the patient (including blood tests or other tests as indicated), use of modern anesthetic agents and local anesthetic blocks (which minimizes the depth of general anesthesia required), and modern anesthetic monitoring equipment. Many patients are awake and standing within 15 to 20 minutes of completion of the procedure and go home the same day.
- While no one can guarantee the outcome of anesthesia, we are trained to provide safe anesthesia and to minimize pain for your pet.
- Every pet is monitored continuously on a multiparameter unit to assess heart rate, respiratory rate, temperature, blood pressure, electrical conductivity of the heart via EKG, and carbon dioxide levels. Changes can be made during the procedure to ensure quality anesthesia that is safe for your pet.
Anesthesia Monitoring Equipment
Can a pet dental be done without anesthesia?
Reasons NOT to use anesthesia-free pet dental cleanings for your dogs or cats:
- A thorough exam and cleaning can’t be done on a dog or cat that is awake. Anesthesia allows us to properly care for your pet’s teeth safely, adequately, and without pain.
- Most oral disease happens below your pet’s gum line and dental x-rays are the only way to identify painful problems such as fractured teeth, periodontal disease, or other problems. Dental x-rays can’t be performed on an awake pet.
- Cleaning and scaling below the gum line are important because it’s where periodontal disease is most active. This can’t be done without anesthesia.
- Anesthesia-free dental cleanings require a pet to be restrained while having their teeth scraped, which is both stressful and likely painful for them.
- There are significantly increasing numbers of pets who, after a number of years of anesthesia-free dental cleanings, have developed severe periodontal disease resulting in multiple extractions or need for extensive treatment.
For more information and to learn the facts about anesthesia-free pet dental cleaning offers we encourage you to visit www.avdc.org/AFD, a site specifically for pet owners and their questions about their pet’s dental health.
At Lake County Veterinary Clinics we are strongly against anesthesia-free dental cleanings and are committed to educating the public about the risks to their pets. A proper pet dental cleaning should always be performed by a veterinarian and involve safe anesthesia and dental radiographs.
Read the AVDC Position on Dental Scaling Without Anesthesia here.